Yoga & health
For many, the journey into yoga begins with a desire for flexibility or stress relief. However, the intersection of yoga and health encompasses far more than touching your toes or taking a deep breath. It is a sophisticated dialogue between movement, anatomy, and the nervous system. Whether you are navigating chronic back pain, recovering from an injury, or simply trying to understand why your body feels different after the age of 40, understanding the science behind the practice is essential for long-term well-being.
This resource acts as a comprehensive guide to bridging the gap between ancient practices and modern health concerns. We move beyond the aesthetics of poses to explore how specific movements, breathing techniques, and recovery strategies influence your physiology. From the microscopic behavior of your fascia to the complex signaling of your gut-brain axis, here is what you need to know to build a sustainable, health-focused practice.
Nervous System Regulation: Beyond Simple Relaxation
In our modern, high-paced environment, the nervous system is often stuck in a state of chronic activation. This goes beyond feeling “stressed”; it manifests physically as burnout, digestion issues, and the paradoxical feeling of being “wiredbuttired.” Understanding how to use yoga to regulate these states is a cornerstone of health.
The Science of Rest and Breathwork
Not all relaxation techniques work for every physiological state. For instance, forcing yourself to sit still in meditation when you are highly activated can sometimes be destabilizing rather than calming. Similarly, breathwork is a powerful tool, but it requires nuance. While deep, slow breathing generally activates the parasympathetic nervous system (the “restanddigest” mode), certain techniques involving breath retention or rapid breathing can trigger anxiety in those with asthma or panic disorders.
- Restorative Yoga: Ideal for deep fatigue where active movement feels depleting. It signals safety to the body by supporting the joints completely.
- Pranayama (Breath Control): Techniques must be chosen based on your current energy. Energizing breaths can combat lethargy, while lengthening the exhalation is key for anxiety reduction.
- Savasana Anxiety: If you feel anxious when lying still, it often indicates a nervous system that perceives stillness as a threat. Gradual exposure and guided techniques are more effective here than forced silence.
Injury Management and Safe Recovery
One of the most common misconceptions is that yoga is purely gentle and risk-free. However, without proper understanding of biomechanics, injuries can occur or recur. Conversely, yoga can be a potent rehabilitative tool when combined with physiotherapy principles.
Navigating Pain: Yoga, Physio, and Massage
When dealing with issues like hamstring strains or chronic lower back pain, the question often arises: should you rest completely or keep moving? Current evidence suggests that complete rest can sometimes delay recovery by causing tissue weakness. Instead, active recovery and modification are key. However, knowing when to seek professional help is crucial.
Complementary therapies like massage play a vital role, but choosing the right type matters:
- Deep Tissue Massage: Beneficial for breaking down adhesions but can cause soreness that mimics injury if done too aggressively or too frequently.
- Sports Massage: Focuses on performance and recovery, often better for active individuals with specific muscle tightness.
- Remedial Therapy: Often the best choice for specific desk-job tension or repetitive strain injuries.
The goal is to integrate these therapies with a modified yoga practice that respects your body’s current limitations while maintaining mobility.
The Invisible Anatomy: Fascia, Proprioception, and Joints
To truly understand stiffness and mobility, we must look beyond the muscles. Two critical components often dictate how we move and feel: fascia and proprioception.
Fascia: The Web of Connection
Fascia is the connective tissue that encases your muscles and organs. Often, what feels like “tightmuscles” is actually dehydrated or matted fascia. Unlike muscle, which responds well to rhythmic contraction, fascia responds better to hydration, varied movement, and sometimes, sustained gentle pressure (like Yin Yoga) or foam rolling. However, aggressive rolling can cause inflammation, highlighting the need for a gentle, consistent approach.
Proprioception and Balance
Proprioception is your body’s ability to sense where it is in space. As we age, or if we don’t challenge it, this sense diminishes, leading to poor posture, ankle sprains, and an increased risk of falls. Complex movements in yoga that require balance and coordination are not just “tricks”; they are essential calibration exercises for your brain and nervous system to maintain physical independence.
Digestive Health and the Microbiome
Emerging research highlights the fascinating link between the gut and the brain, and how yoga might influence this relationship. The gut microbiome affects mood, immunity, and inflammation. Chronic stress—which yoga helps reduce—can negatively alter the bacteria in your gut.
Practices that involve gentle twisting and diaphragmatic breathing can mechanically stimulate the digestive organs and improve motility. However, it is important to distinguish between normal fluctuations (like travel-related digestion changes) and symptoms requiring medical testing. Over-reliance on supplements or extreme detoxes can sometimes disrupt the delicate balance of your microbiome, whereas consistent stress management and moderate movement offer long-term support.
Healthy Aging and Longevity
Why do some people retain mobility into their 70s while others struggle with stiffness in their 40s? The answer often lies in functional mobility and how we address the natural aging process of joints.
After the age of 40, joint stiffness can increase due to changes in synovial fluid and cartilage. However, movement is the lotion that lubricates these joints. The key is adaptation:
- Strength with Flexibility: Flexibility without strength creates instability, which is dangerous for older joints. Yoga practice must evolve to include stability work.
- Functional Tests: The ability to move from standing to sitting on the floor (and back up) without using hands is a strong predictor of longevity and physical independence.
- Morning Stiffness: distinguishing between normal “startupstiffness” and signs of arthritis allows for early intervention and appropriate modification of practice.
Adapting Practice for Life Stages
A rigid approach to yoga—doing the same sequence every day regardless of how you feel—is a recipe for burnout and injury. A health-focused approach prioritizes adaptability.
Pregnancy and Postpartum
The body undergoes massive physiological changes during pregnancy. Deep twists and certain core engagements become contraindicated, while other movements become essential for labor preparation. Postpartum recovery, particularly after a C-section, requires a patient rebuilding of the core, far beyond simple crunches.
The Cycle of Consistency
Whether you are a night owl trying to force a morning practice, or someone recovering from burnout, the “nopain,
nogain” mentality often backfires. Gentle consistency often yields better health markers than sporadic intensity. Understanding your chronotype (natural sleep rhythm) and respecting your energy levels is not laziness; it is intelligent health management.

Why Can Some 70-Year-Olds Move Better Than Some 40-Year-Olds?
The ability to move well into your 70s and beyond is not determined by chronological age, but by the quality and consistency of your daily “movement diet.” Functional decline is often a result of inactivity and narrow movement patterns, not…
Read more
Why Does Your Regular Yoga Teacher Say They Cannot Teach You Now That You Are Pregnant?
The “no” from your yoga teacher isn’t a rejection of your ability, but a necessary shift in focus from intensity to integrity to protect your changing body. Your practice must now prioritize creating space and stability over achieving deep poses,…
Read more
Why Might Gentle Practices Deliver Better Long-Term Results Than Intense Training?
Contrary to the ‘no pain, no gain’ mantra, the key to lifelong fitness lies not in intensity, but in the intelligent, neurological, and structural adaptations fostered by gentle, consistent movement. Intense training can elevate stress hormones, while gentle practices are…
Read more
Why Might Your Yoga Practice Actually Change Your Gut Bacteria?
Your yoga practice is a powerful tool for actively modulating your gut microbiome, with measurable changes happening in as little as three days. Yoga reduces stress-induced inflammation and “leaky gut” by calming the gut-brain axis. It stimulates the vagus nerve,…
Read more
Why Does Your Digestion Change When You Travel Even If You Eat the Same Foods?
The digestive upset you feel when traveling isn’t just about the food; it’s your gut’s sensitive internal ecosystem reacting to a major disruption in its communication with your brain. Chronic stress from travel elevates inflammatory signals, altering the composition of…
Read more
Why Does Your Chest Rise When You Breathe Even Though You Try to Belly Breathe?
Your inability to stop chest breathing isn’t a lack of focus; it’s often a physical ‘lock’ caused by deep-seated muscular tension and neurological patterns. Chronic tension, especially in the hip flexors, can physically tether your diaphragm, restricting its natural movement….
Read more
Why Can’t You Relax Even When You Finally Have Time Off?
Your inability to relax isn’t a willpower issue; it’s a physiological signal that your nervous system is stuck in survival mode. Burnout isn’t just exhaustion but an accumulation of incomplete “stress cycles” that keep your body on high alert. Forcing…
Read more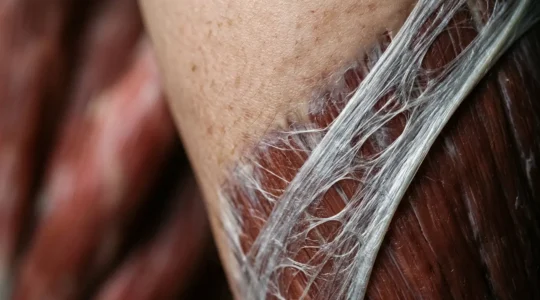
Why Does Stretching Never Seem to Release That Stubborn Tightness in Your IT Band?
That persistent tightness you’re fighting isn’t a stubborn muscle; it’s a restriction in your body’s fascial web, and it requires a completely different approach than stretching. Fascia is a dense, innervated tissue that gives the body shape but can become…
Read more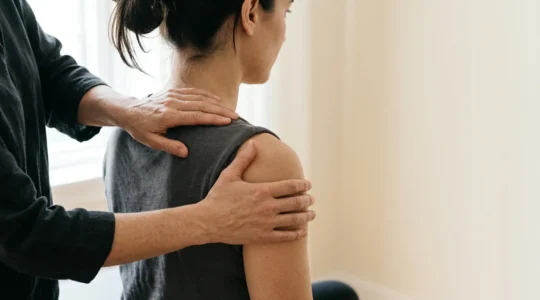
Why Do Your Shoulders Retense Within Hours After a Massage?
The stubborn return of muscle tension isn’t a failure of the massage or your ability to relax; it’s a fundamental misunderstanding of the tissue involved. Your pain isn’t just in the muscle; it’s locked in the fascial web, a tough…
Read more
Why Does Your Neck Still Hurt After Weeks of Foam Rolling It Every Day?
Constant foam rolling isn’t working because your neck pain is rarely a neck problem—it’s a symptom of a systemic imbalance that rolling the sore spot can actually make worse. Much of what you feel as “tightness” is actually “protective tension,”…
Read more