That persistent tightness you’re fighting isn’t a stubborn muscle; it’s a restriction in your body’s fascial web, and it requires a completely different approach than stretching.
- Fascia is a dense, innervated tissue that gives the body shape but can become “stuck” due to dehydration, trauma, or repetitive stress.
- Unlike elastic muscle, fascia responds to slow, sustained pressure (90+ seconds) which allows its gel-like ground substance to “melt” and become more fluid.
Recommendation: Stop aggressively stretching the area. Instead, learn to apply gentle, sustained compression to the surrounding tissues to encourage a fascial release and restore fluid movement.
If you’ve ever found yourself relentlessly stretching a tight iliotibial (IT) band, only to feel the same stubborn, unyielding tension return hours later, you are not alone. It’s a common frustration among athletes and desk workers alike. You follow the conventional wisdom: you stretch, you foam roll, you endure the discomfort, yet the relief is fleeting, if it comes at all. This cycle can lead you to believe you’re simply not flexible or that the tightness is a permanent fixture of your anatomy.
The common approach focuses almost exclusively on the muscle, treating it as an isolated, elastic band that simply needs to be pulled longer. But this overlooks the master controller of our structural integrity: the fascia. This intricate, three-dimensional web of connective tissue wraps, supports, and permeates every muscle, bone, nerve, and organ in your body. It’s the silent architecture that dictates your posture, movement patterns, and, crucially, your sensations of tightness.
What if the key wasn’t to force the tissue into submission with more aggressive stretching, but to understand its unique language? The truth is, fascial restrictions don’t respond to the same rules as muscle tissue. This is not a failure of your efforts, but a failure of the technique. Your body isn’t broken; it’s simply misunderstood.
This guide will illuminate the true nature of your chronic tightness. We will dissect the difference between muscle, fascial, and nerve tension, reveal why conventional stretching fails for fascial issues, and outline the precise techniques that encourage genuine, lasting release. Prepare to shift your perspective from fighting your body to intelligently communicating with it.
To navigate this complex inner landscape, this article provides a clear roadmap. We will explore the nature of fascia, differentiate between types of tightness, and detail the specific methods required for effective release, culminating in a practical plan to maintain your fascial health.
Summary: Why Stretching Fails Your IT Band and What to Do Instead
- What Is Fascia and Why Does It Get Stiff Even When Your Muscles Are Flexible?
- How Can You Tell if Your Tightness Is Muscle, Fascia or Nerve Tension?
- Why Fascial Release Needs Different Techniques Than Muscle Stretching?
- The Fascia Release Mistake That Causes Inflammation Instead of Freedom
- How to Build a Weekly Fascial Health Practice That Prevents Future Restrictions?
- What Happens Inside Your Joints When Stiffness Creeps in After Your 40s?
- Relaxation Massage or Remedial Therapy: Which Do You Actually Need for Desk Job Tension?
- How to Choose Between Sports Massage and Deep Tissue When You Have Chronic Back Pain?
What Is Fascia and Why Does It Get Stiff Even When Your Muscles Are Flexible?
Think of fascia not as a series of separate parts, but as a single, continuous, three-dimensional web that provides your body with its form and structure. It’s like a full-body suit worn underneath the skin. While your muscles are the engines that create movement, the fascia is the wiring harness, the support chassis, and the communication network all in one. Contemporary research shows that fascia plays a significant role in everything from force transmission and proprioception to pain generation.
This tissue isn’t just inert packing material; it is a dynamic sensory organ. As researchers have noted, it is densely populated with nerve endings. This explains why fascial restrictions can be so painful and why a dysfunctional fascial system can send confusing pain signals throughout the body.
Fascia is not inert but richly innervated. Thoracolumbar fascia contains free nerve endings, Ruffini corpuscles, and sympathetic fibers.
– Slater et al., Frontiers in Neurology
So why does it get stiff? Unlike a muscle that contracts and relaxes, fascia gets stiff when it becomes dehydrated, inflamed, or “stuck.” After an injury, repetitive movement (like sitting at a desk), or emotional stress, the smooth, sliding layers of fascia can adhere to each other. The gel-like substance between its fibers, called ground substance, loses its fluidity and becomes more like glue. This is why you can have full muscular flexibility in one test, yet feel a deep, burning, or pulling restriction that a simple stretch just can’t reach. You’re not stretching a muscle; you’re pulling against a densely woven, dehydrated, and adhered network.

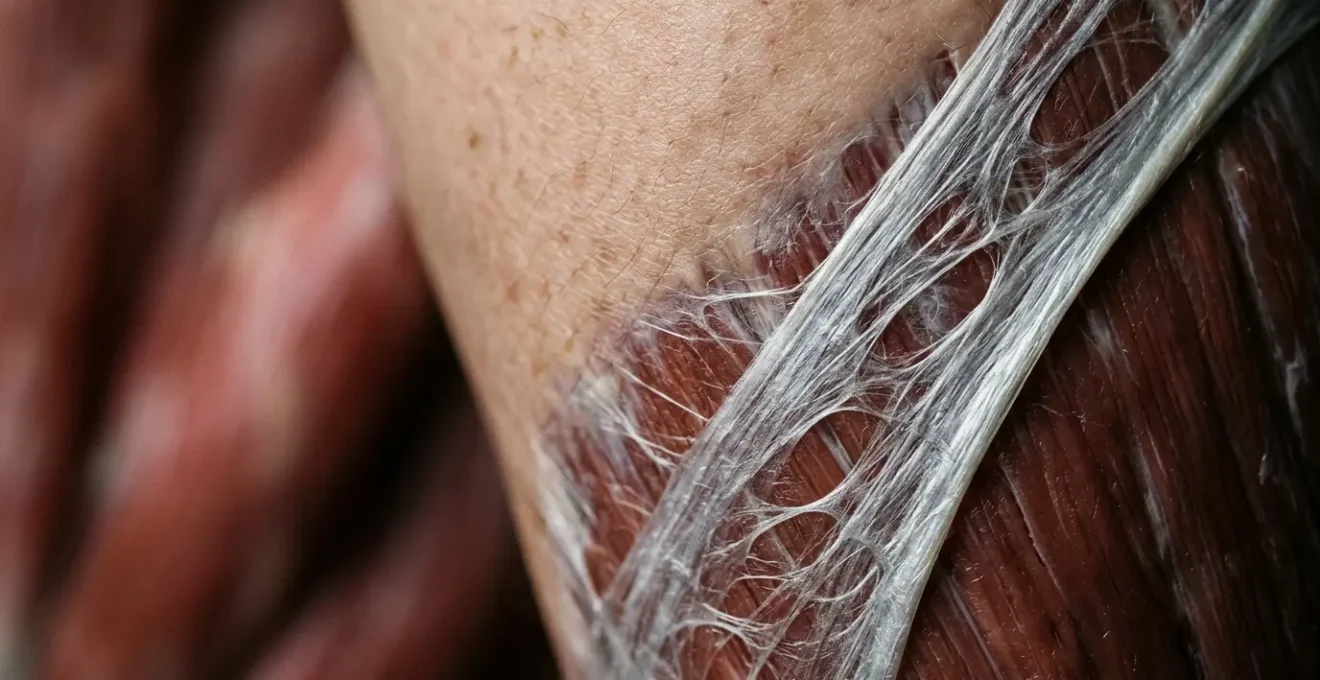
As this image illustrates, fascia is an incredibly intricate structure. The stiffness you feel is not a simple knot but a complex architectural problem within this fibrous matrix. To solve it, you must address the health of the entire web, not just pull on one strand.
How Can You Tell if Your Tightness Is Muscle, Fascia or Nerve Tension?
The first step toward effective treatment is accurate diagnosis. Not all tightness is created equal, and your body uses different sensations to signal the origin of the problem. Treating a nerve issue with aggressive muscle techniques, for example, can significantly worsen the situation. The key is to become a detective of your own internal sensations. Is the feeling a dull ache, a sharp electric line, or a tough, leathery restriction?
Muscle tightness typically feels like a dull, aching, or tired sensation. It’s often localized to the belly of a specific muscle that has been overworked. This type of tightness usually responds well to rest, warmth, and gentle stretching; you feel a “good stretch” and notice immediate, albeit sometimes temporary, improvement in your range of motion.
Fascial restriction, on the other hand, presents very differently. It’s often described as a burning, pulling, or searing sensation. The area can feel tough, dense, and unyielding, like trying to stretch a piece of leather. When you try to stretch it, you hit a hard “end point” with little give. You might also notice that the restriction follows a broad plane or line, rather than being confined to a single muscle belly. This is the “stubborn” tightness of the IT band that doesn’t yield.
Nerve tension is the sharpest and most alarming of the three. It is characterized by sensations of tingling, electricity, numbness, or a sharp, radiating pain that travels along a defined path, like down the back of your leg (sciatica). Stretching a tense nerve to its end range will almost always aggravate the symptoms, causing a sharp increase in pain or tingling. This is a clear signal to stop and seek professional assessment.
The following chart, based on clinical observations and an understanding of tissue behavior, provides a clear guide to help you differentiate these sensations. Pay close attention to not just what you feel, but how the feeling responds to movement and stretching.
| Tissue Type | Sensation Quality | Response to Stretching | Location Pattern |
|---|---|---|---|
| Muscle Tightness | Dull ache, tiredness, heaviness | Improves after warm-up and gentle stretching | Localized to specific muscle belly |
| Fascial Restriction | Burning, pulling, stuck sensation, gritty texture | Barely changes with quick stretching | Along fascial lines and bands |
| Nerve Tension | Sharp, electric, tingling, radiating | Aggravated by end-range stretching | Follows nerve distribution patterns |
Why Fascial Release Needs Different Techniques Than Muscle Stretching?
The fundamental reason stretching fails to release stubborn fascia lies in the physical properties of the tissue itself. A muscle is designed to be elastic; it’s like a rubber band. It responds well to being lengthened and then returning to its resting state. Fascia, however, is not primarily elastic. It is a viscoelastic and thixotropic material. This means its texture and viscosity can change in response to pressure and temperature, much like honey or silly putty.
When you perform a quick, 30-second stretch, you are engaging the elastic qualities of the muscle. This does very little to affect the dense, semi-solid state of restricted fascia. To create change in the fascial web, you need to engage its thixotropic properties. This requires two key ingredients: sustained pressure and time. You need to apply gentle, consistent pressure to a restricted area and simply wait. This sustained input signals the nervous system to relax its guarding, and the warmth and pressure begin to change the ground substance from a thick, gel-like state to a more fluid, liquid one. This “melting” allows the layers of tissue to slide freely once again.
Scientific research backs this up. To induce a change in the fascia, the input needs to be held for a significant duration. As a 2024 study published in Scientific Reports found that only interventions lasting 90-120 seconds induce adaptive responses to the pressure applied during self-myofascial release. Bouncing or holding a stretch for a mere 30 seconds simply doesn’t provide enough time for the fascial matrix to remodel.
Case Study: The Thixotropic “Melt” in Action
The power of targeting fascia’s thixotropic nature is clearly demonstrated in clinical research. For example, a randomized controlled trial on plantar fasciitis patients showed that foam rolling was effective not just by “stretching” but by changing the tissue’s physical state. The sustained friction and pressure from the roller generated warmth, which helped to break up fibrous adhesions. This warming effect directly influenced the thixotropic property of the plantar fascia, making it more pliable and restoring its natural extensibility. The result was a measurable improvement in range of motion and a reduction in pain, all by treating the tissue according to its unique physical properties.
This is the paradigm shift: stop trying to pull the fascia apart and start thinking about how to melt it. Techniques like Myofascial Release, using tools like foam rollers or massage balls correctly (i.e., slowly and patiently), or receiving hands-on therapy are all designed around this principle of sustained, intelligent compression.
The Fascia Release Mistake That Causes Inflammation Instead of Freedom
In the quest to release stubborn tightness, it’s easy to adopt a “more is better” mentality. If a little pressure is good, then a lot of pressure must be great, right? This is the single most common and detrimental mistake in self-myofascial release: using excessive, aggressive force. When you grind a foam roller into your IT band with all your body weight, causing excruciating pain, you are not releasing the fascia. You are brutalizing it.
Remember, fascia is a sensitive, innervated tissue. When you apply aggressive pressure, your nervous system perceives it as a threat. It responds by reflexively tightening the muscles and fascia around the area to protect it—the exact opposite of your goal. You are essentially starting a fight with your own body, and your nervous system will always win that fight.
As one clinic specializing in fascial work warns, this aggressive approach can be counterproductive and even harmful.
When you apply excessive pressure through foam rolling, you risk causing microtrauma to the fascia. This can lead to inflammation, irritation, and even more tightness, which is the opposite of what you’re trying to achieve.
– Myofascial Release Mississauga, Clinical perspective on foam rolling risks
The goal is not to crush the tissue but to coax it. A gentle, sustained pressure that is just enough to engage the tissue without causing a pain response is far more effective. This gentle approach allows the nervous system to feel safe, which permits the tissue to “melt” and release. In fact, research on foam rolling’s physiological mechanisms reveals that constant but manageable tension on soft tissues is what increases local blood flow and helps modulate inflammation, promoting healing rather than causing more damage.

The correct technique should feel like a “good pain”—an intense but tolerable sensation of release, not a sharp, wince-inducing agony. You should be able to breathe deeply and relax into the pressure. If you find yourself gritting your teeth and holding your breath, you have gone too far. Back off the pressure until you find that therapeutic sweet spot. True release comes from listening to your body, not shouting at it.
How to Build a Weekly Fascial Health Practice That Prevents Future Restrictions?
Resolving fascial restrictions is one thing; preventing them from returning is another. True fascial health is not about a single, intense session but about integrating small, consistent habits into your weekly routine. The goal is to keep the fascial web hydrated, mobile, and pliable, so adhesions don’t get a chance to form in the first place. A proactive approach is always more effective than a reactive one.
First, prioritize hydration. Fascia is primarily composed of water. When you are dehydrated, the ground substance becomes thicker and stickier, increasing friction between tissue layers. Simply ensuring you drink enough water throughout the day is a foundational and often overlooked aspect of fascial health.
Second, embrace movement variability. Fascia adapts to the loads and positions you place on it. If you spend eight hours a day in the same seated posture, your fascia will remodel itself to support that shape, leading to tightness in the hip flexors and weakness in the glutes. Counteract this by introducing varied movements: take short walking breaks, do simple stretches at your desk, or try activities like yoga, tai chi, or dancing that move your body through multiple planes of motion.
Finally, schedule dedicated “fascial hygiene” sessions. This doesn’t need to be an hour-long ordeal. Just 10-15 minutes, two to three times a week, can make a significant difference. During this time, use a foam roller, massage ball, or your own hands to slowly scan your body for areas of emerging tightness. When you find a tender spot, follow the principles we’ve discussed: sink in with gentle, sustained pressure, wait for the tissue to melt, and breathe. This is not a workout; it’s a conversation with your body.
Action Plan: Your Weekly Fascial Health Audit
- Hydration Check: At the start of the week, set a realistic daily water intake goal. Track it for three days. Is your tissue getting the basic hydration it needs to stay slick and mobile?
- Identify Sticky Spots: Take 5 minutes to slowly move and stretch. Scan your body from head to toe. Where do you feel the first signs of restriction or “stuckness”? Note the top 3 areas that need attention.
- Schedule “Melt” Sessions: Block out two 15-minute slots in your calendar for the week. Treat them like appointments. This is your dedicated time to apply sustained pressure to the sticky spots you identified.
- Incorporate Movement Snacks: Plan one 5-minute “movement snack” for each workday. This could be a walk around the office, a few cat-cow stretches, or simply standing up and reaching overhead. The goal is to break up static postures.
- Conduct a Sensation Audit: At the end of the week, reflect on the sensations in your body. Have the sticky spots changed? Do you feel more fluid? This feedback loop is crucial for refining your practice.
What Happens Inside Your Joints When Stiffness Creeps in After Your 40s?
The increased stiffness many people experience as they enter their 40s and beyond isn’t just “in your head.” It’s the result of tangible, physiological changes within your connective tissues and joints. One of the primary culprits is a gradual decline in the body’s production of a remarkable molecule: hyaluronic acid (HA).
Hyaluronic acid is a key component of your body’s ground substance—the lubricating, gel-like material that fills the spaces within your fascial matrix. It is also a major component of synovial fluid, the viscous liquid that lubricates your joints. HA’s superpower is its ability to attract and hold vast amounts of water, giving tissues their plumpness, hydration, and, most importantly, their ability to slide and glide without friction.
As we age, our cells become less efficient at producing HA. As a 2025 systematic review published in the Journal of Cosmetic Dermatology confirms that aging reduces the production of hyaluronic acid in the skin and connective tissues. This decline has a direct, cascading effect on our movement. With less HA, the ground substance becomes less viscous and more “sticky.” The fascial layers, which once glided effortlessly over each other, now experience more friction. In the joints, the synovial fluid thins, offering less cushioning and lubrication.
The result? That familiar feeling of morning stiffness, creaky joints, and a reduced sense of fluidity in your movements. It takes longer to “warm up” because your tissues are literally drier and more resistant to movement. This isn’t just about muscles getting tighter; it’s about the entire internal environment becoming less lubricated. This makes a consistent fascial health practice, which promotes hydration and circulation within the tissues, even more critical as we age to counteract these natural degenerative processes.
Relaxation Massage or Remedial Therapy: Which Do You Actually Need for Desk Job Tension?
Desk job tension is a universal complaint, but it manifests in different ways. Sometimes it’s a generalized feeling of stress and tightness in the neck and shoulders. Other times, it’s a specific, recurring knot under the shoulder blade that triggers headaches. The key to effective treatment is understanding that these are two different problems requiring two different solutions: relaxation massage and remedial therapy.
Think of it as the difference between a software problem and a hardware problem. Relaxation massage is a “software” reboot for your nervous system. Its primary goal is to down-regulate a stressed nervous system. Using long, flowing, rhythmic strokes, it calms the “fight or flight” response, reduces levels of the stress hormone cortisol, and addresses the global, stress-induced tension that makes your entire upper back feel tight. It’s the perfect choice when you feel overwrought, mentally exhausted, and physically tense all over after a stressful week.
Remedial therapy, which includes modalities like deep tissue or trigger point therapy, is a “hardware” repair. It is a problem-solving approach. A remedial therapist begins with an assessment to pinpoint the specific biomechanical issue—the adhesion, trigger point, or fascial restriction that is causing your chronic pain pattern. The treatment is targeted, focusing on releasing that specific structure to restore proper function. This is the right choice when you have a persistent, localized issue, like that one knot on your right side that always flares up and refers pain to your neck.
Neither is “better” than the other; they simply have different goals. Choosing the wrong one can lead to frustration. If you have a specific, stubborn knot and you get a relaxation massage, you might feel relaxed, but the knot will likely still be there. Conversely, if you’re feeling stressed and overwhelmed and you get an intense remedial session, it could be too much for your already frazzled nervous system. The following table breaks down the key differences to help you make an informed choice.
| Feature | Relaxation Massage | Remedial Therapy |
|---|---|---|
| Primary Goal | Down-regulate nervous system, reduce global stress-induced tension | Problem-solve specific biomechanical issue or chronic pain pattern |
| Session Structure | Full-body flow, consistent rhythm, calming environment | Begins with assessment (postural, range of motion), targeted treatment |
| Analogy | System reboot for stressed nervous system ‘software’ | Hardware repair for faulty component (adhesion, trigger point) |
| Best For Desk Workers | Neck feels tight everywhere after stressful week | Specific recurring knot on one side causing headaches |
| Pressure Style | Moderate, soothing, rhythmic | Varies from gentle to firm based on tissue response |
Key Takeaways
- Your stubborn tightness is often a fascial restriction, not a muscular one, which is why traditional stretching is ineffective.
- Fascia is a thixotropic material that responds to slow, sustained pressure (90+ seconds), not quick or aggressive force. It needs to “melt,” not be stretched.
- Aggressive foam rolling creates inflammation and causes the nervous system to guard the tissue, making the problem worse. Gentle, patient pressure is far more effective.
How to Choose Between Sports Massage and Deep Tissue When You Have Chronic Back Pain?
When grappling with chronic back pain, navigating the world of massage therapy can be confusing. Two terms that often come up are “sports massage” and “deep tissue massage.” While they both can involve firm pressure, their philosophies, applications, and goals are distinct. Choosing the right one depends on the nature and cause of your chronic pain.
Deep tissue massage is a modality specifically designed to address chronic pain and postural issues. Its primary focus is on releasing adhesions and “knots” in the deeper layers of muscle and fascia. A therapist will work slowly and deliberately, using firm pressure to target specific areas of restriction that have built up over time due to injury, repetitive stress, or poor posture. The goal is structural: to break down scar tissue and restore normal movement. Indeed, a study on mobility physical therapy outcomes found that when combined with stretching, deep tissue massage can significantly enhance range of motion and improve function in patients with chronic pain.
Sports massage, while it may incorporate deep tissue techniques, has a broader and more function-oriented scope. It is typically tailored to the specific needs of an athlete or an active individual. It can be used pre-event to stimulate muscles, post-event to aid recovery and reduce soreness, or as part of a maintenance program to improve flexibility and prevent injury. A sports massage session is often more dynamic, incorporating active and passive stretching, joint mobilization, and quicker-paced techniques alongside deeper work. The focus is less on releasing a single chronic adhesion and more on optimizing the performance of the entire musculoskeletal system for a particular activity.
So, which is right for your chronic back pain? If your pain stems from long-term postural strain (like sitting at a desk) or an old injury that has created deep-seated adhesions, a course of deep tissue massage is likely the more direct and effective starting point. If your back pain is related to your active lifestyle or a specific sport, and you’re looking to improve performance and prevent future flare-ups, a regular sports massage might be the better long-term strategy. Ultimately, the best approach is to communicate clearly with a qualified therapist who can assess your specific condition and blend techniques to best suit your needs.
Now that you understand the true nature of your fascial tissue and the specific methods required to release it, the path to relief is clear. The next logical step is to move from theory to practice. Begin by gently exploring the techniques discussed, using a foam roller or massage ball not as an instrument of torture, but as a tool for communication. Find a tender area, apply gentle pressure, and wait patiently for the “melt.” This is the beginning of a new, more intelligent relationship with your body.