
The stubborn return of muscle tension isn’t a failure of the massage or your ability to relax; it’s a fundamental misunderstanding of the tissue involved. Your pain isn’t just in the muscle; it’s locked in the fascial web, a tough connective tissue that requires slow, sustained pressure and consistent frequency to truly change. This guide explains how to shift from temporary muscle relief to permanent fascial release for lasting freedom from tension.
It’s a frustratingly common cycle. You leave the massage table or yoga mat feeling weightless, the chronic tension in your shoulders and neck finally gone. You feel fluid, relaxed, and renewed. But within hours, or by the next morning, that familiar, stubborn knot begins to creep back in, tightening its grip. It feels like all the money and time you invested simply evaporated. You blame your posture, your stress, or even the therapist, but the root cause is deeper and more misunderstood than you think.
The conventional wisdom about stretching, hydration, and “just relaxing” only scratches the surface. These approaches primarily target your muscles, which are designed for quick responses. However, the deep, persistent tension that defines your discomfort isn’t just muscular. It’s held within your body’s extensive network of connective tissue, the fascia.
The truth is, you’ve been trying to solve a deep-seated structural problem with superficial solutions. True, lasting release doesn’t come from a single, intense session but from understanding the unique language your fascia speaks. It’s a language of time, patience, and consistency.
This article will deconstruct the cycle of returning tension. We will explore the critical difference between sensory relaxation and true tissue release, examine the specific timelines and techniques your body needs to change, and reveal why the frequency of your practice matters more than its intensity. It’s time to stop chasing temporary relief and start building a foundation for profound, lasting release.
To navigate this deep dive into the science of tension release, here is a breakdown of the key areas we will explore.
Summary: Unlocking Lasting Relief from Chronic Tension
- What Is the Difference Between Feeling Relaxed and Your Muscles Actually Releasing?
- How Long Must You Hold a Stretch Before Deep Tissue Actually Starts Changing?
- Yin Yoga, Restorative or Monthly Massage: Which Creates the Deepest Tissue Release?
- Why Forced Relaxation Creates More Tension 24 Hours Later
- What Room Temperature, Lighting and Sound Allow Deepest Physical Relaxation?
- The Error of Monthly Massages When Weekly Sessions Could Resolve Your Issue in 8 Weeks
- Why Fascial Release Needs Different Techniques Than Muscle Stretching?
- Why Does Stretching Never Seem to Release That Stubborn Tightness in Your IT Band?
What Is the Difference Between Feeling Relaxed and Your Muscles Actually Releasing?
The blissful, “jelly-like” state you feel after a great massage is primarily a nervous system response. This is the sensation of being relaxed. Your therapist’s skilled touch, the calm environment, and the focused attention all signal to your brain that it’s safe to power down your fight-or-flight response. Your sympathetic nervous system (the “accelerator”) yields to the parasympathetic nervous system (the “brake”). This process lowers stress hormones, slows your heart rate, and tells your muscles to stop guarding.
As experts from the JSNP Health Science Team note, this is a core benefit of bodywork:
Massage therapy works to counteract chronic stress by inducing a relaxation response that calms the central nervous system and alleviates stress-induced symptoms.
– JSNP Health Science Team, The Science Behind Massage Therapy: How It Works on Muscles and the Nervous System
However, this neurological state of relaxation is not the same as a structural release. A true release involves a physical change in the resting length and texture of your connective tissues, particularly the fascia. Fascia is the dense, fibrous web that encases and connects every muscle, bone, and organ in your body. Chronic tension, poor posture, and repetitive movements cause this web to become dehydrated, stiff, and “glued down” in certain areas. This is the source of that deep, unyielding knot.
While a relaxed nervous system makes the muscles more pliable and receptive, it does not, by itself, break down these tough fascial adhesions. That requires a different kind of input—one focused on time and sustained pressure. So, while you may feel relaxed, the underlying structural issue that creates the tension pattern remains, ready to reassert itself as soon as you return to your daily stressors and movement habits.
How Long Must You Hold a Stretch Before Deep Tissue Actually Starts Changing?
If you’ve ever held a stretch for 30 seconds and wondered why it didn’t “fix” your tightness, you’re not alone. The reason is simple: you haven’t given your deep tissue enough time to respond. Quick, bouncy stretches or short holds primarily affect the more elastic muscle fibers. But to influence the tough, collagen-rich fascia, you need to apply a sustained, low-load pressure.
This is where the process of mechanotransduction comes in. It’s a biological phenomenon where cells convert mechanical signals (like sustained pressure) into chemical responses. For fascia, this process is slow. Practitioners in the field of myofascial release suggest a minimum hold time of 90 to 120 seconds. It’s only after this initial period that the dense, gel-like ground substance of the fascia begins to soften, allowing the collagen fibers to realign, rehydrate, and release their grip.
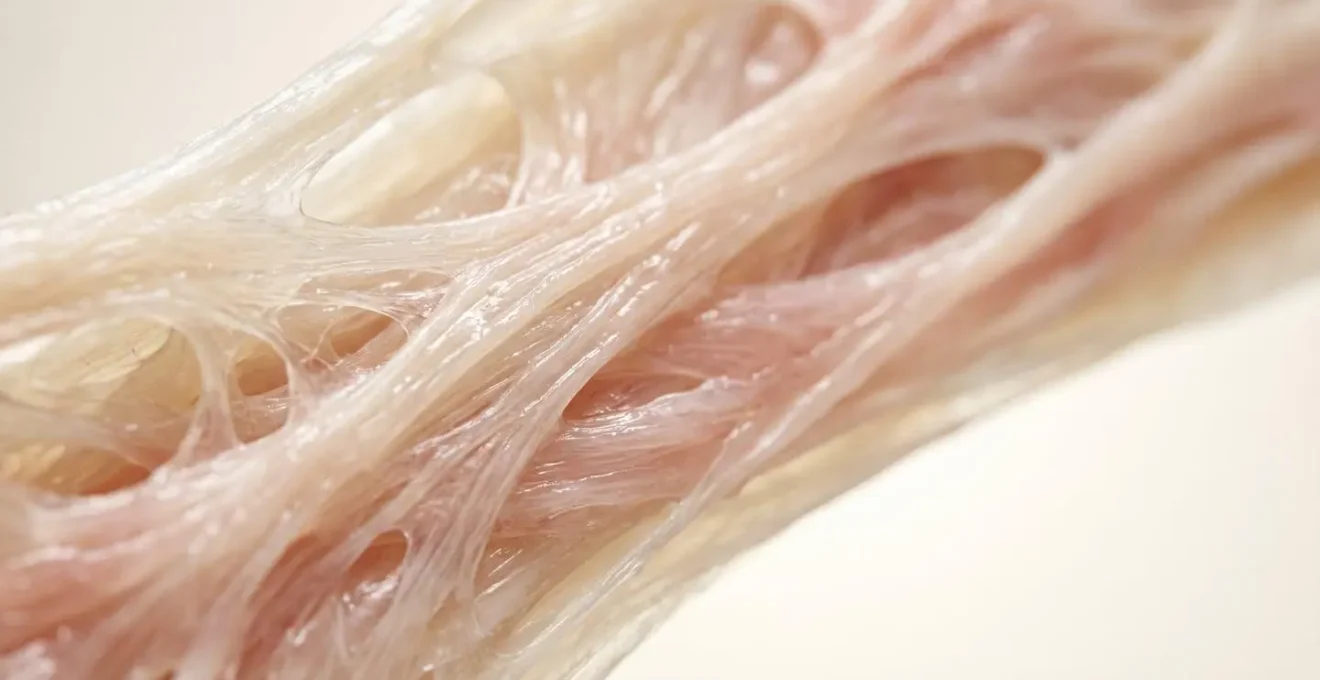
Anything less than this 90-second threshold is often just a conversation with your muscles and nervous system. It’s the long, patient hold that allows you to speak directly to the connective tissue itself. Recent scientific inquiry is beginning to validate this long-held therapeutic principle. A study found that while short dynamic stretching didn’t change tissue stiffness, a 5-minute static stretch was shown to reduce both muscle and fascia stiffness, a first-of-its-kind finding demonstrating real mechanical changes in the fascia itself.
Think of it like trying to melt a frozen block of honey. A quick blast of heat won’t do much. You need to apply gentle, consistent warmth over time for it to slowly turn from a solid into a fluid. Your fascia is that honey; it doesn’t respond to force, but it yields to patience.
Yin Yoga, Restorative or Monthly Massage: Which Creates the Deepest Tissue Release?
With the understanding that time is the secret ingredient for fascial release, we can evaluate common wellness practices with a more critical eye. Not all relaxation is created equal when the goal is deep, structural change. Let’s compare three popular modalities: Restorative Yoga, a monthly massage, and Yin Yoga.
Restorative Yoga is a practice of profound stillness and support. Using props like bolsters and blankets, the body is placed in positions of complete comfort. Its primary goal is to activate the parasympathetic nervous system, creating deep sensory and mental relaxation. While incredibly beneficial for stress, it doesn’t typically involve the sustained, specific pressure needed to remodel fascia.
A monthly massage can provide targeted pressure, but its effectiveness for lasting change is limited by frequency. A 60-minute session once a month is often just enough to calm the nervous system and temporarily relieve muscle soreness. By the time the next session comes around, the fascial restrictions have likely reformed, forcing the therapist to start from square one. It’s a maintenance pattern, not a corrective one.
Yin Yoga stands out as a practice specifically designed to target the fascial matrix. It achieves this through its two core principles: long-held postures and muscular relaxation. By holding floor-based poses for 3 to 7 minutes, practitioners apply that crucial low-load, sustained stress to the deep connective tissues. According to research on the topic, this duration is what stimulates the cells within the fascia (fibroblasts) to begin the mechanotransduction process of remodeling. As Yoga Journal’s experts confirm, “The long-held stretches of Yin yoga are a strong way to target large areas of fascia.”
While a skilled manual therapist can achieve profound fascial release, the consistent, self-directed practice of Yin Yoga empowers you to make these changes on your own schedule, creating a cumulative effect that a monthly appointment struggles to match.
Why Forced Relaxation Creates More Tension 24 Hours Later
Have you ever laid on a massage table, acutely aware of a tense muscle, and tried with all your might to “let it go”? You command your shoulder to drop, you mentally try to soften the area, but it only seems to get tighter. This phenomenon, known as paradoxical tension, highlights a critical flaw in how we approach release: you cannot force relaxation.
Relaxation is not an act of doing; it is an act of non-doing. When you try to force a muscle to release, you are engaging your mind and your will. This very effort is a form of tension. You are sending a command from your brain, which is a sympathetic (fight-or-flight) nervous system activity. This creates a conflicting signal in your body: one part of your nervous system is receiving a relaxing stimulus (the massage), while another is actively engaged in a task (“I must relax this muscle!”).
This internal conflict can lead to a rebound effect. The muscle may temporarily yield under the therapist’s pressure, but the underlying neurological “guarding” pattern has been reinforced, not released. Your nervous system interprets this forceful self-command as a subtle form of stress. The next day, as the immediate sensory pleasure of the massage fades, that underlying neurological tension re-emerges, often feeling even more pronounced than before.
True release happens when the nervous system feels safe enough to let go on its own. It’s an invitation, not a command. Instead of forcing, the goal is to create the conditions for release to occur naturally. This involves shifting your focus away from the tense area and towards something neutral, like the sensation of your breath, the feeling of the table supporting you, or the ambient sounds in the room. By disengaging the “doing” mind, you allow the parasympathetic “braking” system to take over organically, leading to a much deeper and more authentic state of release that lasts.
What Room Temperature, Lighting and Sound Allow Deepest Physical Relaxation?
Creating an environment that signals safety to the nervous system is not an indulgence; it’s a non-negotiable prerequisite for deep tissue release. Your body will not and cannot let go of deep-seated tension if it perceives any threat—subtle or overt—in its surroundings. Temperature, lighting, and sound are three of the most powerful tools for communicating safety to your primal brain.
Temperature: A cool room is a major obstacle to relaxation. When you’re cold, your body’s natural response is to tense up and shiver to generate heat. This is a survival mechanism. For fascia to become more pliable and for muscles to relax, they need warmth. The ideal room temperature is one where you feel comfortably warm without being hot, typically between 72-76°F (22-24°C). Warmth not only prevents protective tensing but also has a direct physiological effect on stress hormones. In fact, research demonstrates that consistent heat application can significantly decrease levels of the stress hormone cortisol.
Lighting: Bright, overhead, or blue-toned light is a powerful signal to your brain that it’s daytime and time to be alert. This type of lighting stimulates cortisol production and suppresses melatonin, the hormone of rest. To facilitate deep relaxation, the lighting should be low, indirect, and warm-toned (like candlelight or a salt lamp). Dim light signals to the nervous system that it’s time to wind down, making it much easier to transition into a parasympathetic state. Complete darkness can be even more effective for some, as it removes all visual stimuli.

Sound: Sudden, loud, or jarring noises trigger an immediate startle response, sending a jolt of adrenaline through your system. The ideal soundscape for relaxation is one that is either completely silent or consists of consistent, non-intrusive, low-frequency sounds. This could be a white noise machine, ambient music without a discernible melody or lyrics, or the sound of gentle rain. These predictable, monotonous sounds have a lulling effect on the brain, helping it to disengage from analytical thought and sink into a deeper state of rest.
The Error of Monthly Massages When Weekly Sessions Could Resolve Your Issue in 8 Weeks
For those caught in the cycle of chronic tension, the monthly massage often feels like a necessary ritual. It provides a brief window of relief, but it rarely solves the underlying problem. The fundamental error in this approach lies in a misunderstanding of dosage and the cumulative nature of therapeutic bodywork. A monthly session is often a strategy of maintenance, not resolution. It’s like trying to get in shape by going to the gym once a month—the benefits of one session have completely worn off by the time the next one arrives.
Lasting change in the body’s soft tissues, especially the dense fascial network, requires consistency. Each session builds upon the last. A single massage can reduce inflammation and calm the nervous system, but these effects are temporary. A more frequent dosage creates a powerful cumulative effect that begins to retrain the body’s patterns. For instance, a 2014 clinical trial found that 60-minute massages 2-3 times per week were significantly more effective for chronic neck pain than less frequent sessions.
The true power of frequency is in its ability to produce fundamentally different biological responses, as demonstrated by a compelling study on the effects of repeated massage.
Case Study: The Cumulative Biological Effects of Massage Frequency
A 5-week study with 139 participants showed that the frequency of massage profoundly changes its biological impact. Participants receiving once-weekly massage showed sustained improvements in their immune response. However, those receiving massage twice-weekly experienced distinct neuroendocrine changes, including an increase in oxytocin (the “bonding” hormone) and a decrease in cortisol and vasopressin (stress-related hormones). The conclusion was stark: the “dose” of massage creates profoundly different outcomes. A higher frequency doesn’t just provide *more* of the same benefit; it provides a *different* and potentially more transformative benefit for chronic stress patterns.
This suggests that an intensive series of weekly or twice-weekly sessions over a focused period (e.g., 8 weeks) could create the neuro-fascial breakthrough needed to resolve a chronic issue. Once the pattern is broken and the tissue has been remodeled, you can then transition to a less frequent, maintenance schedule. The initial investment in frequency is what allows for the long-term resolution that a monthly massage can never achieve.
Why Fascial Release Needs Different Techniques Than Muscle Stretching?
For decades, stretching has been the default prescription for tightness. However, this advice is based on a muscle-centric view of the body. When the root of stubborn tightness lies in the fascia, traditional muscle stretching is often ineffective or even counterproductive. This is because muscle and fascia are fundamentally different tissues with different properties, and they respond to different stimuli.
Muscle tissue is elastic, vascular (rich in blood supply), and designed for contraction and relaxation. It benefits from dynamic movements and a variety of stretches that increase its flexibility and blood flow. It responds relatively quickly.
Fascia, on the other hand, is a dense, collagen-based connective tissue. It is primarily avascular (having a poor blood supply), making its healing and adaptation processes much slower. As the Fascia Research Group explains, its cellular nature dictates a completely different approach:
Fascia is avascular, dense connective tissue, rich in collagen. It’s designed for stability. Its cellular nature dictates that it responds to sustained pressure and low-load tension, not the rapid contract-relax cycles that benefit muscles.
– Fascia Research Group, Fascial or Muscle Stretching? A Narrative Review
Furthermore, fascia is incredibly rich in nerve endings. In fact, anatomical research reveals that deep fascia can have a threefold higher nerve density than the underlying muscles it covers. It is a major sensory organ, communicating information about pressure, pain, and position (proprioception) directly to the central nervous system. This is why fascial adhesions can be such a potent source of chronic pain. Trying to force a release in this highly sensitive tissue with aggressive, short-duration muscle stretching can cause it to tense up defensively.
Fascial release techniques, therefore, rely on patience. They use sustained pressure (from a therapist’s hands, a ball, or in a long-held yoga pose) to slowly “melt” the ground substance of the fascia, allowing fibers to glide more freely. It’s a dialogue with the nervous system, not a battle for length.
Key takeaways
- Lasting relief comes from targeting fascia, not just muscle, which requires slow, sustained holds (90+ seconds).
- The frequency of treatment is more critical than intensity; a short, concentrated series of sessions is more effective for chronic issues than monthly maintenance.
- True relaxation is a state of nervous system safety; it cannot be forced and requires a supportive environment (warmth, dim light, low sound).
Why Does Stretching Never Seem to Release That Stubborn Tightness in Your IT Band?
The iliotibial (IT) band is the poster child for misunderstood tightness. Countless runners, cyclists, and athletes have spent hours painfully rolling and stretching this thick band of tissue on the outside of the thigh, only to find the tightness returns with a vengeance. The reason this approach consistently fails is that it’s based on a flawed premise: that the IT band is a muscle that can be stretched into submission.
In reality, the IT band is not a muscle; it is an incredibly thick, powerful sheet of fascia. It’s as tough as a tire tread, and trying to lengthen it through stretching is biomechanically futile. The “tightness” you feel is rarely the IT band itself becoming shorter. Instead, the tension originates from the muscles that attach to it, primarily the tensor fasciae latae (TFL) at the hip and the gluteus maximus.
When other hip abductor muscles, like the gluteus medius, are weak or underactive, the TFL is forced to overwork to stabilize the pelvis. This chronic over-activation creates massive tension, which then pulls on the IT band, creating the sensation of tightness down the side of the leg. The IT band is the victim, not the culprit. Furthermore, biomechanical studies demonstrate that deep fascia transmits approximately 30% of force generated during muscular contraction, meaning the tension you feel is part of a complex system of force distribution, not an isolated tight spot.
Therefore, stretching the IT band is a waste of time. Painful foam rolling directly on the band can also irritate the highly innervated tissue and the structures underneath it. The solution lies in addressing the root cause: strengthening the weak hip muscles and releasing the tension in the overworked TFL and glutes.
Action Plan: Rethinking Your IT Band Strategy
- Target gluteus medius activation through clamshell exercises to address the root cause of TFL overcompensation.
- Perform lateral band walks to strengthen hip abductors and reduce overall tension pulling on the IT band.
- Incorporate single-leg hip bridges to activate the gluteus maximus, reducing the reliance on the tensor fasciae latae.
- Use a foam roller or therapy ball on the TFL (at the front of your hip) and gluteal muscles—not on the IT band itself—to temporarily reduce hypertonicity.
- Focus on addressing any fascial restrictions around the hip with sustained, low-load pressure rather than aggressive stretching.
The journey to becoming free from chronic tension requires a paradigm shift. It’s time to move away from the frustrating cycle of temporary fixes and adopt a more intelligent, patient, and consistent approach. By understanding the true nature of your body’s tissues and working with them, not against them, you can achieve the profound and lasting release you’ve been searching for.